Genoskin – a French National Center for Scientific Research (CNRS) spinoff – believes there is a better alternative to animal testing when it comes to dermatological and cosmetic research: donated human skin, which it collects from surgical procedures. Keeping the skin ‘alive’ using an ex vivo culture system, the company is able to provide skin samples in the form of slide sections, frozen tissue, or epidermal to hypodermal sections.
“I have previously worked with transgenic and knockout mice to investigate the function of a particular gene in skin development,” explains says Pascal Descargues, CEO of Genoskin. “The mouse models were very useful in discovering new molecular pathways, but we were not able to confirm the results for humans because we were missing key comparable elements. Furthermore, we found that a mouse model reproducing the skin disorder Netherton Syndrome could not be used to screen drugs at all since the disease is lethal for mice.”
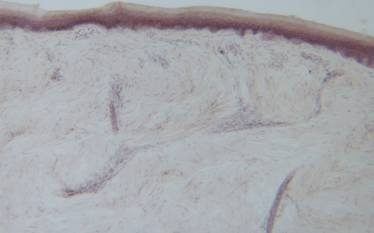
Descargues initially started the Genoskin project during postdoctoral training at the Paul Sabatier University/CRNS to offer more in vitro tools for skin researchers, but ethics were also a consideration. “I was never comfortable with the idea of performing experiments on mice and killing them,” he adds.
Some researchers have turned to lab-grown skin to address the same problems, but Descargues argues that synthetic skin does not offer the same benefits as the real thing. “Reconstructed or bio-printed skin models face many limitations, including immature barrier function, absence of immune cells, no dermal extracellular matrix, no adipose tissues, and the absence of skin appendages like hair follicles. All of which means that synthesized skin may not be as accurate a predictive model for testing parameters, such as dermal absorption, allergies, or for testing sub-cutaneous injections.”
Collecting skin samples requires ethical committee approval, agreements with hospitals, and donor consent, but a small amount of skin can go a long way. In 2016, Genoskin collected 100 skin samples, which they turned into 1000 skin models. “There are more than 20,000 abdominoplasties carried out every year in France alone – and more than 200,000 in the US – and skin could make a real difference to testing. I am convinced that, at least in dermatological and cosmetic research, we could one day replace all animal testing worldwide.”
My fascination with science, gaming, and writing led to my studying biology at university, while simultaneously working as an online games journalist. After university, I travelled across Europe, working on a novel and developing a game, before finding my way to Texere. As Associate Editor, I’m evolving my loves of science and writing, while continuing to pursue my passion for gaming and creative writing in a personal capacity.















